BM(Hons) MD FRCS(Neurosurgery)
Consultant Neurosurgeon

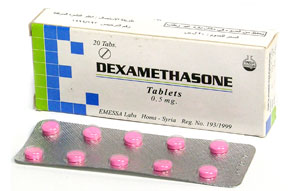
If you have been diagnosed with a (suspected) brain tumour, you are likely to be started on some drug treatments including dexamethasone and often phenytoin.
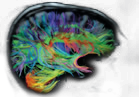
Dexamethasone is a steroid drug that has proven benefit in reducing the swelling (oedema) caused by some brain tumours. Swelling associated with brain tumours may contribute to the symptoms produced by the tumour including headaches and neurological deficits (weakness, loss of speech, etc.). Steroids should, therefore, help to relieve some of these symptoms.
Dexamethasone normally takes 8-24 hours for the first effects to be apparent.
You will often be prescribed a high dose initially (4mg 4 times per day) and this will be reduced following your treatment, as directed by your treating doctors. Depending on your tumour type and your needs for other treatment (e.g. radiotherapy) you may be advised to remain on a small dose. If you have been taking dexamethasone for more than a few days it is very important not to stop it suddenly, rather the dose should be gradually reduced over a period of days.
Every drug has side effects. The more common side effects with dexamethasone are gastritis or stomach ulcers (to prevent this you will be given an anti-acid drug), increased appetite, weight gain, muscle weakness, diabetes, increased risk of infection, and psychological disturbances. Generally the side effects are worse with higher doses given for longer periods of time.
Commonly used drugs for the control of various forms of seizures that may be caused by brain tumours include Lamotrigine | Drugs | BNF | NICE and Levetiracetam | Drugs | BNF | NICE
Other drugs are also occasionally used.
